Report on Government Services 2017
Volume E, Chapter 12
Public hospitals
This chapter reports on the performance of governments in providing public hospitals, with a focus on acute care services.
Download the chapter
- Chapter 12 Public hospitals and attachment tables (PDF - 2979 Kb)
- Chapter 12 Attachment tables (XLSX - 1001 Kb)
- Key Facts
- Indicator Framework
- Indicator Results
- Indigenous Data
Total recurrent expenditure on public hospitals (excluding depreciation) was $55.0 billion in 2014-15. In 2014-15, government real recurrent expenditure on public hospitals was $2321 per person for Australia, up from $1851 in 2010-11.
Funding for public hospitals comes from a number of sources. The Australian, State and Territory governments contributed 90.8 per cent of funding for public hospital services in 2014‑15, with non-government sources contributing 9.2 per cent.
In 2014-15, Australia had 698 public hospitals. Although 68.9 per cent of hospitals had 50 or fewer beds, these smaller hospitals represented only 14.3 per cent of total available beds.
There were approximately 6.0 million separations from public (non-psychiatric) hospitals in 2014-15. Nationally, this translates into 239.8 separations per 1000 people. Acute separations accounted for the majority of separations from public hospitals.
A total of 33.8 million individual service events were provided to non-admitted patients in public hospitals in 2014-15. There were 7.4 million presentations to emergency departments in 2014-15.
Public hospitals aim to alleviate or manage illness and the effects of injury and rehabilitate where necessary by providing universal access to acute, non and sub-acute care along with emergency, outpatient and community care that is:
- timely, affordable and accessible
- appropriate and responsive to the needs of individuals and communities
- high quality and safe
- well co-ordinated to ensure continuity of care where more than one service type, and/or ongoing service provision is required
- sustainable in terms of workforce, infrastructure, innovation and capacity to respond to emerging needs.
Governments aim for public hospital services to meet these objectives in an equitable and efficient manner.
The performance indicator framework provides information on equity, efficiency and effectiveness, and distinguishes the outputs and outcomes of public hospitals. The performance indicator framework shows which data are complete and comparable in the 2017 Report.
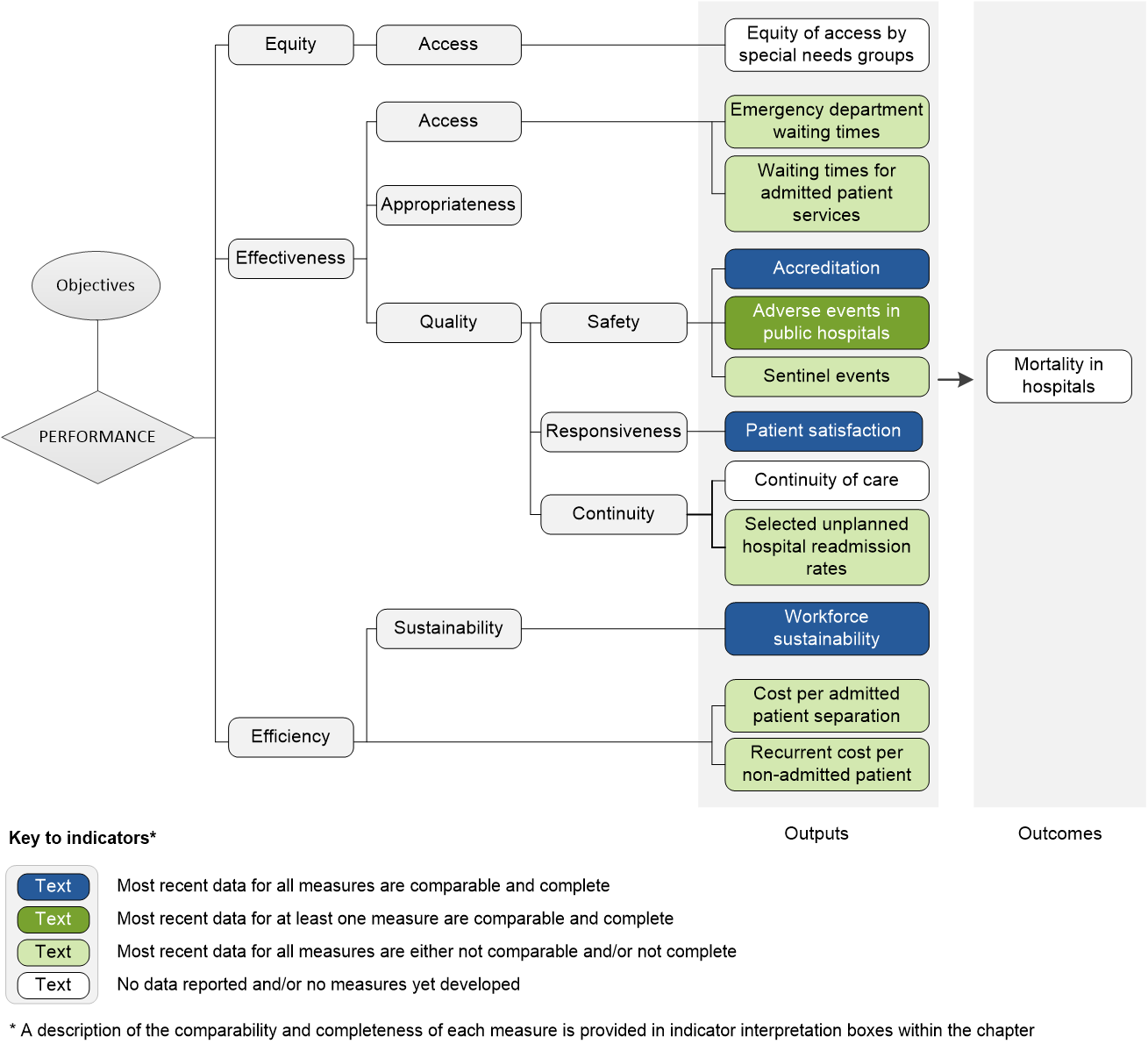
An overview of the Public hospitals performance indicator results are presented. Information to assist the interpretation of these data can be found in the indicator interpretation boxes in the Public hospitals chapter and attachment tables.
Effectiveness — Access indicators
Emergency department waiting times
Emergency department waiting times by triage category — proportion of patients seen on time, 2015-16 (%)
| Triage category | NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust |
|---|---|---|---|---|---|---|---|---|---|
| Resuscitation | 100 | 100 | 100 | 100 | 100 | 100 | na | 100 | 100 |
| Emergency | 82 | 78 | 74 | 77 | 70 | 80 | na | 63 | 77 |
| Urgent | 76 | 71 | 61 | 53 | 56 | 59 | na | 53 | 67 |
| Semi-urgent | 80 | 72 | 74 | 67 | 70 | 64 | na | 60 | 74 |
| Non-urgent | 94 | 89 | 94 | 93 | 92 | 87 | na | 89 | 93 |
| Total | 81 | 74 | 70 | 65 | 66 | 66 | na | 61 | 74 |
Length of stay for emergency department care, proportion of patients staying for four hours or less, 2015‑16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| % | 74.8 | 71.2 | 75.2 | 76.0 | 66.0 | 66.3 | na | 63.6 | 73.2 |
Waiting times for admitted patient services
Overall elective surgery waiting times, 2015-16 (days waited)
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| 50th percentile | 55 | 30 | 29 | 30 | 40 | 72 | na | 29 | 37 |
| 90th percentile | 328 | 174 | 163 | 161 | 233 | 452 | na | 229 | 260 |
Presentations to emergency departments with a length of stay of 4 hours or less ending in admission, public hospitals (per cent), 2015-16
| Triage category | NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust |
|---|---|---|---|---|---|---|---|---|---|
| Resuscitation | 52 | 57 | 59 | 66 | 59 | 58 | na | 46 | 57 |
| Emergency | 45 | 53 | 56 | 58 | 45 | 34 | na | 28 | 50 |
| Urgent | 41 | 51 | 55 | 48 | 40 | 24 | na | 25 | 47 |
| Semi-urgent | 46 | 55 | 58 | 50 | 47 | 28 | na | 28 | 50 |
| Non-urgent | 66 | 65 | 65 | 60 | 67 | 48 | na | 36 | 64 |
| Total | 44 | 53 | 56 | 51 | 44 | 28 | na | 27 | 49 |
Effectiveness — Quality — Safety indicators
Accreditation
Proportion of accredited public hospitals, 30 June 2015
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| % | 98 | 91 | 95 | 94 | 90 | 61 | 100 | 100 | 93 |
Adverse events in public hospitals
Selected healthcare-associated infections in acute care hospitals, per 10 000 patient days, 2015-16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| rate | 0.7 | 0.7 | 0.7 | 0.9 | 0.7 | 0.9 | 0.8 | 0.6 | 0.7 |
Adverse events treated in hospitals, per 100 separations, 2014-15
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Rate | 6.8 | 6.6 | 6.4 | 7.1 | 7.5 | 8.0 | 7.3 | 3.5 | 6.7 |
Falls resulting in patient harm in public hospitals, per 1000 separations, 2014-15
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Rate | 5.6 | 3.6 | 3.7 | 5.0 | 5.0 | 6.9 | 4.5 | 1.8 | 4.5 |
Sentinel events
Adverse events occurring due to hospital system and process deficiencies that result in death of, or serious harm to, a patient, 2014-15
Effectiveness — Quality — Responsiveness indicators
Patient satisfaction
Proportion (%) of persons who went to an emergency department in the last 12 months reporting that:
ED doctors, specialists or nurses always or often listened carefully to them, 2015-16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Doctors/specialists | 86.2 | 86.7 | 87.5 | 90.0 | 84.5 | 84.4 | 81.5 | 90.9 | 87.0 |
| Nurses | 87.8 | 91.2 | 91.9 | 91.2 | 87.3 | 91.8 | #88.4 | 88.9 | 90.3 |
ED doctors, specialists or nurses always or often showed respect to them, 2015-16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Doctors/specialists | 88.6 | 88.6 | 88.9 | 88.7 | 86.4 | 85.7 | 81.8 | 92.0 | 88.3 |
| Nurses | 89.5 | 92.2 | 93.6 | 91.4 | 87.1 | 91.8 | #86.8 | 88.9 | 91.5 |
ED doctors, specialists or nurses always or often spent enough time with them, 2015-16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Doctors/specialists | 81.6 | 83.9 | 86.2 | 86.7 | 80.6 | 83.7 | 74.8 | 90.3 | 83.6 |
| Nurses | 84.5 | 87.4 | 90.2 | 90.4 | 82.6 | 89.2 | #79.0 | 89.1 | 87.1 |
Proportion (%) of persons who were admitted to hospital in the last 12 months reporting that:
Hospital doctors, specialists or nurses always or often listened carefully to them, 2015-16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Doctors/specialists | 92.3 | 93.0 | 92.8 | 93.2 | 90.1 | 89.9 | #85.1 | #91.9 | 92.2 |
| Nurses | 90.7 | 92.1 | 93.5 | 94.3 | 88.7 | 90.7 | 85.5 | 88.9 | 92.0 |
Hospital doctors, specialists or nurses always or often showed respect to them, 2015-16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Doctors/specialists | 91.3 | 92.9 | 93.2 | 94.1 | 92.3 | 90.6 | 87.5 | 93.9 | 92.5 |
| Nurses | 90.3 | 94.2 | 93.6 | 94.3 | 90.9 | 93.3 | 86.7 | 88.8 | 92.6 |
Hospital doctors, specialists or nurses always or often spent enough time with them, 2015-16
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| Doctors/specialists | 88.3 | 90.0 | 90.8 | 89.3 | 86.7 | 84.6 | 81.0 | #87.5 | 88.9 |
| Nurses | 89.7 | 90.3 | 92.2 | 91.0 | 86.8 | 89.6 | 85.7 | 89.4 | 90.2 |
Source: Attachment tables 12A.46–49
Effectiveness — Quality — Continuity indicators
Selected unplanned hospital readmission rates
Rate at which patients unexpectedly return to hospital within 28 days for further treatment of the same condition (per 1000 separations), 2014-15
| Surgical procedure prior to separation | NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust |
|---|---|---|---|---|---|---|---|---|---|
| Knee replacement | 19.4 | 19.4 | 36.3 | 28.1 | 18.6 | 18.3 | 7.0 | np | 22.7 |
| Hip replacement | 16.9 | 16.1 | 23.5 | 16.7 | 7.1 | 21.6 | 8.5 | np | 17.1 |
| Tonsillectomy and adenoidectomy | 31.7 | 26.0 | 49.5 | 41.3 | 53.9 | 34.9 | 31.3 | 105.0 | 35.7 |
| Hysterectomy | 28.6 | 28.4 | 40.9 | 38.6 | 25.5 | 27.5 | 78.3 | np | 31.6 |
| Prostatectomy | 23.0 | 23.4 | 33.0 | 12.6 | 13.0 | – | np | np | 24.3 |
| Cataract surgery | 2.5 | 2.9 | 5.1 | 3.1 | 2.5 | 4.1 | 0.9 | 10.1 | 3.1 |
| Appendicectomy | 20.5 | 19.8 | 23.9 | 35.1 | 26.7 | 36.5 | 14.3 | 37.7 | 22.0 |
Source: Attachment table 12A.50
Efficiency — Sustainability indicators
Workforce sustainability
Nursing workforce by age group (per cent), 2015
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| <30 | 15.8 | 18.1 | 16.0 | 16.9 | 14.6 | 13.6 | 16.7 | 18.1 | 16.5 |
| 30–39 | 20.7 | 21.7 | 21.0 | 21.2 | 19.8 | 16.6 | 23.7 | 27.1 | 21.0 |
| 40–49 | 23.2 | 24.1 | 26.0 | 24.9 | 24.7 | 24.0 | 25.0 | 21.9 | 24.3 |
| 50–59 | 27.2 | 24.9 | 26.3 | 25.9 | 29.4 | 33.2 | 24.2 | 22.7 | 26.5 |
| 60+ | 13.1 | 11.2 | 10.8 | 11.1 | 11.4 | 12.6 | 10.4 | 10.3 | 11.6 |
Medical practitioner workforce by age group (per cent), 2015
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| <30 | 9.1 | 10.5 | 9.6 | 10.1 | 9.5 | 9.6 | 8.2 | 10.9 | 9.7 |
| 30–39 | 26.2 | 28.5 | 28.7 | 30.0 | 27.2 | 23.2 | 27.7 | 36.9 | 27.8 |
| 40–49 | 24.4 | 23.4 | 25.9 | 25.8 | 24.4 | 25.5 | 25.3 | 23.6 | 24.6 |
| 50–59 | 20.4 | 20.2 | 20.8 | 19.5 | 21.0 | 23.1 | 22.5 | 16.3 | 20.4 |
| 60+ | 20.0 | 17.4 | 15.0 | 14.5 | 17.8 | 18.6 | 16.3 | 12.4 | 17.4 |
Efficiency indicators
Cost per admitted patient separation
Recurrent cost per weighted separation, 2014-15
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| $ | 4 943 | 4 442 | 4 897 | 6 124 | 5 708 | 5 165 | 6 637 | 6 734 | 5 025 |
Capital cost per weighted separation, 2014-15
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| $ | 901 | 867 | 548 | 1 120 | 763 | 765 | 1 075 | 608 | 818 |
Source: Attachment table 12A.57
Recurrent cost per non-admitted patient
Average cost per non-admitted acute emergency department presentation, 2014-15
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| $ | 377 | 392 | 531 | 577 | 500 | 398 | 578 | 497 | 449 |
Average cost per non-admitted service event, 2014-15
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
|---|---|---|---|---|---|---|---|---|---|
| $ | 205 | 273 | 340 | 315 | 364 | 243 | 242 | 445 | 272 |
Source: Attachment table 12A.61
Notes
These data and caveats for these data are available in chapter 12 and attachment 12A.
# Proportion has a margin of error >10 percentage points which should be considered when using this information.
na Not available. – Nil or rounded to zero. np Not published.
| Table number | Table title |
|---|---|
| Table 12A.15 | Patients treated within national benchmarks for emergency department waiting time, by Indigenous status, by State and Territory |
| Table 12A.20 | Waiting times for elective surgery in public hospitals, by Indigenous status and procedure, by State and Territory (days) |
| Table 12A.36 | Separations for falls resulting in patient harm in hospitals, per 1000 separations, 2014-15 |
| Table 12A.51 | Unplanned hospital readmission rates, by Indigenous status, hospital peer group, remoteness and SEIFA IRSD quintiles, 2014-15 |