Report on Government Services 2026
PART E, SECTION 13: RELEASED ON 5 FEBRUARY 2026
13 Services for mental health
This section reports on the Australian, state and territory governments’ provision of services for mental health. Performance reporting focuses on state and territory governments’ specialised mental health services, and services for mental health subsidised under the Medicare Benefits Schedule (Medicare) (provided by General Practitioners (GPs), psychiatrists, psychologists and other allied health professionals).
Content advisory
If you, or someone you know, is experiencing crisis, visit your nearest hospital emergency department or use any of the crisis helplines below.
If life is in immediate danger please call 000.
The Indicator results tab uses data from the data tables to provide information on the performance for each indicator in the Indicator framework. The same data is also available in CSV format.
Data downloads
- 13 Services for mental health data tables (Excel - 791.1 KB)
- 13 Services for mental health dataset (CSV - 2.7 MB)
Refer to the corresponding table number in the data tables for detailed definitions, caveats, footnotes and data source(s).
Context
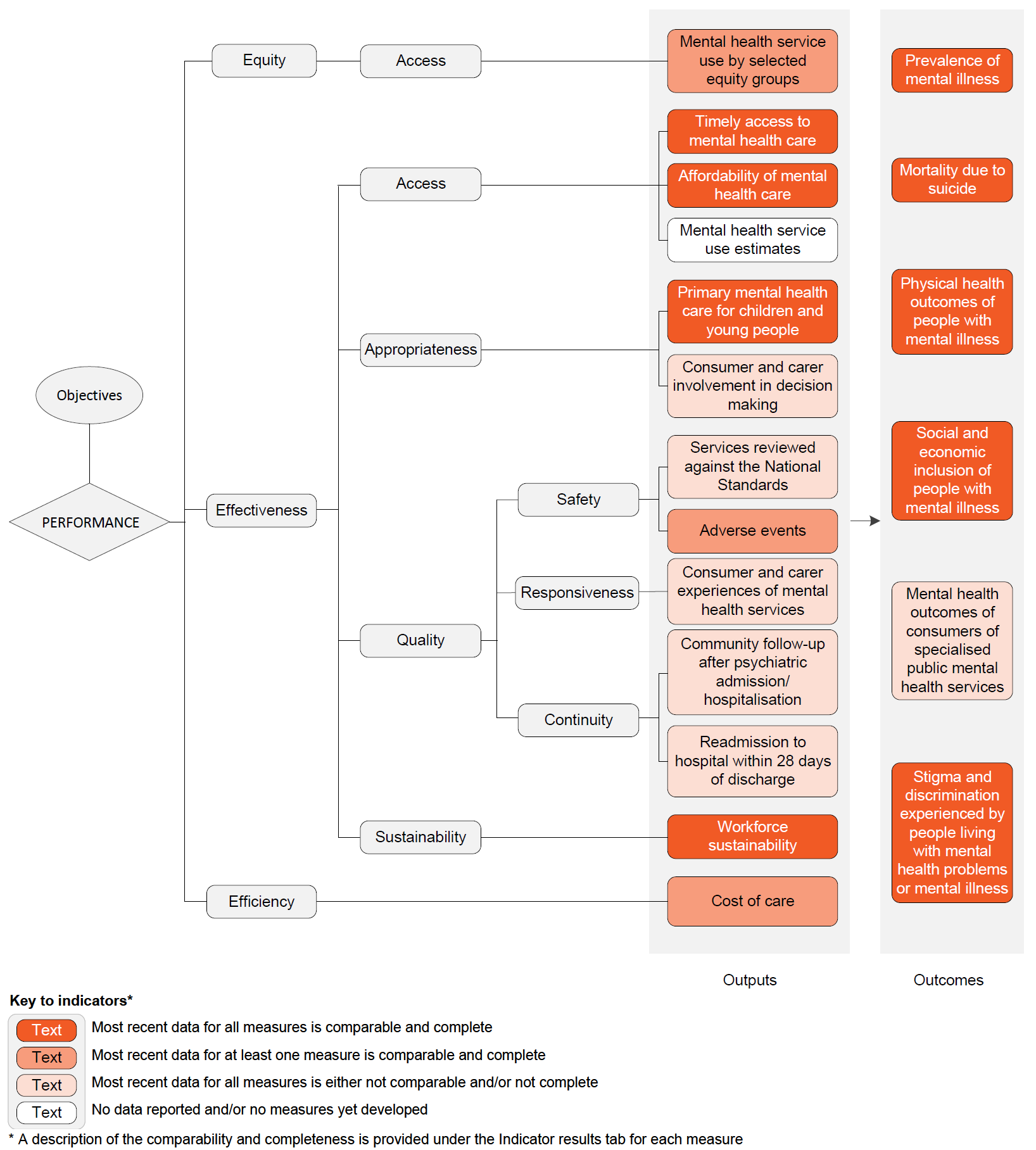
Objectives for services for mental health
Services for mental health aim to:
- promote mental health and wellbeing, and where possible prevent the development of mental health problems, mental illness and suicide, and
- when mental health problems and illness do occur, reduce the impact (including the effects of stigma and discrimination), promote recovery and physical health and encourage meaningful participation in society, by providing services that:
- are high quality, safe and responsive to consumer and carer goals
- facilitate early detection of mental health issues and mental illness, followed by appropriate intervention
- are coordinated and provide continuity of care
- are timely, affordable and readily available to those who need them
- are sustainable.
Governments aim for services for mental health to meet these objectives in an equitable and efficient manner.
The World Health Organization describes positive mental health as:
… a state of wellbeing that enables people to cope with the stresses of life, realise their abilities, learn and work well, and contribute to their community (WHO 2025).
Mental illness refers to a diverse range of behavioural and psychological conditions that can affect an individual’s mental health, functioning and quality of life. Each condition is unique in its incidence across the lifespan, causal factors and treatments.
A range of services are provided or funded by Australian, state and territory governments to meet the needs of people with mental health issues. The key services are:
- Medicare‑subsidised mental health specific services that are partially or fully funded under Medicare on a fee‑for‑service basis and are provided by GPs, psychiatrists, psychologists or other allied health professionals under specific mental health items.
- State and territory government specialised mental health services (treating mostly low prevalence, but severe, mental illnesses), which includes:
- Admitted patient care in public hospitals – specialised services provided to inpatients in standalone psychiatric hospitals or psychiatric units in general acute hospitals. While not a state and territory government specialised mental health service, this section also reports on emergency department presentations for mental health-related care needs
- Community‑based public mental health services, comprising:
- ambulatory care services and other services dedicated to assessment, treatment, rehabilitation and care, and
- residential services that provide beds in the community, staffed onsite by mental health professionals.
- Not-for-profit, non‑government organisation (NGO) services, funded by the Australian, state and territory governments focused on providing wellbeing, support and assistance to people who live with a mental illness. These include crisis, support and information services such as Beyond Blue, Lifeline, Kids Helpline, and 13YARN.
- The National Disability Insurance Scheme (NDIS), which began full roll out in July 2016. People with a psychiatric disability who have significant and permanent functional impairment are eligible to access funding through the NDIS. In addition, people with a disability other than a psychiatric disability may also be eligible for funding for mental health-related services and support if required.
- The Australian, state and territory governments also share a focus on prevention and early intervention through suicide prevention programs and investment to reduce gaps in care (including emphasising a whole of system approach and the role of social determinants of health on people’s mental health and wellbeing).
Other services (for example, specialist homelessness services) provided and/or funded by governments play a significant role in supporting people with mental illness but are not specialised or specific mental health services. Information on these services can be found in the Mental Health section of the Australian Institute of Health and Welfare (AIHW) website (AIHW 2025).
State and territory governments are responsible for funding, delivering and/or managing specialised services for mental health including inpatient/admitted care in hospitals, community‑based ambulatory care and community‑based residential care.
The Australian Government is responsible for overseeing and funding of a range of services for mental health and programs that are primarily provided or delivered by private practitioners or NGOs. These include:
- Medicare‑subsidised services provided by GPs (under both general and specific mental health items)
- private psychiatrists and other allied mental health professionals
- Pharmaceutical Benefits Scheme (PBS) funded mental health‑related medications and other programs designed to prevent suicide or increase the level of social support, and
- community‑based care for people with a mental illness and their carers.
The Australian Government also funds state and territory governments for health services through the approaches specified in the National Mental Health and Suicide Prevention Agreement1 (the Agreement) and the National Health Reform Agreement (NHRA) which includes a mental health component.
Under the Agreement, the Australian, state and territory governments are jointly responsible for a number of areas including:
- mental health workforce planning, training and accreditation
- mental health promotion, prevention, early intervention and social and emotional wellbeing programs, suicide prevention and stigma reduction
- help and crisis hotlines
- psychosocial support services for people who are not supported through the NDIS
- contributions to the National Agreement on Closing the Gap (reducing suicide of Aboriginal and Torres Strait Islander people towards zero, ensuring all government funded services are culturally safe and responsive, and building a strong, sustainable community‑controlled sector).
The Agreement expires in June 2026. The Productivity Commission delivered the Review of the National Mental Health and Suicide Prevention Agreement in November 2025 (PC 2025). Key recommendations include that:
- the current Agreement should be extended to June 2027 to allow sufficient time for co-design of a new policy architecture
- the renewed policy architecture should include a Mental Health Declaration to set a long-term vision, a five-year national agreement to tackle short-term priorities, and new governance, accountability and funding structures to support whole-of-government action
- the independence and responsibilities of the National Mental Health Commission should be formalised
- separate schedules to the next Agreement should be included for services for Aboriginal and Torres Strait Islander people, services distinctly focused on suicide prevention, and services for people experiencing co-occurring problematic use of alcohol and other drugs and mental ill health and/or suicidal distress.
A number of other national initiatives and nationally agreed strategies and plans underpin the delivery and monitoring of services for mental health in Australia including:
- the National Suicide Prevention Strategy 2025–2035 (DHDA 2025)
- the National Mental Health Workforce Strategy 2022–2032 (DHDA 2023).
- National Mental Health and Suicide Prevention Agreement, 2022 https://federalfinancialrelations.gov.au/agreements/mental-health-suicide-prevention-agreement Locate Footnote 1 above
Nationally in 2023‑24, total recurrent expenditure on mental health was around $13.8 billion or $511.39 per person (table 13A.1; figure 13.1). State and territory governments contributed the majority ($9.0 billion or 65.3%, which includes Australian Government funding under the NHRA), with Australian Government expenditure of $4.8 billion (table 13A.1).
Expenditure on Medicare‑subsidised services was the largest component of Australian Government expenditure on services for mental health in 2023-24 ($1.6 billion or 32.4%). This comprised Medicare‑payments for psychologists and other allied health professionals (16.2%), consultant psychiatrists (9.8%) and GP services (6.4%). The Australian Government also spent $733.4 million in 2023‑24 on mental health-related medications under the PBS (15.3% of total Australian Government expenditure) (table 13A.2).
Nationally in 2023-24, expenditure on admitted patient services was the largest component of state and territory governments’ expenditure on specialised mental health services ($3.8 billion or 41.3%), followed by expenditure on community‑based ambulatory services ($3.5 billion or 38.6%) (table 13A.3). State and territory governments’ expenditure on specialised mental health services, by source of funds and depreciation (which is excluded from reporting) and per person in the population is in tables 13A.4, 13A.5 and 13A.6, respectively.
In 2023-24, 10.6% of the total population received Medicare/DVA services, with 1.8% of the total population receiving state and territory government specialised mental health services (figure 13.2). The proportion of the population using state and territory government specialised mental health services and Medicare/DVA services has remained relatively constant over time. Service use per person increased for all service types across the time series, however GPs remain the most commonly accessed service provider (table 13A.7).
Information on the proportion of new clients who accessed state and territory governments’ specialised and Medicare-subsidised services for mental health is available in tables 13A.8–9.
For the first time, the 2021 Census collected information on diagnosed long‑term health conditions. Over two million people (2,231,543) reported having a diagnosed long‑term mental health condition (ABS 2022).
Medicare‑subsidised services for mental health
In 2024‑25, 9.6 million Medicare‑subsidised services for mental health were provided by psychologists (clinical and other services) (6.2 million), psychiatrists (2.8 million) and other allied health professionals (0.6 million). GPs provided a further 3.6 million Medicare‑subsidised specific services for mental health. Service usage rates varied across states and territories (table 13A.10).
GPs are often the first service accessed by people seeking help when suffering from a mental illness. They can diagnose, manage and treat mental illnesses and refer patients to more specialised service providers. According to the Royal Australian College of General Practitioners, mental health was the most common reason patients visited their GP, for the ninth consecutive year (RACGP 2025).
State and territory governments’ specialised mental health services
Across states and territories, the mix of admitted patient services, community‑based services, and care types differs. As the unit of activity varies across these three service types, service mix differences can be partly understood by considering items which have comparable measurement such as expenditure (table 13A.3), numbers of full-time equivalent (FTE) direct care staff (table 13A.11), accrued mental health patient days (table 13A.12) and mental health beds (table 13A.13).
Additional data is also available on the most common principal diagnoses for admitted patients, community‑based ambulatory contacts by age group and specialised mental health care by Indigenous status in the Mental Health section of the AIHW website (AIHW 2025).
Crisis and support organisations
Crisis, support and information services such as Beyond Blue, Lifeline and Kids Helpline are provided to support Australians experiencing mental health issues. In 2024-25:
- Lifeline received 1,063,635 calls and answered 844,791 calls.
- 13YARN received 27,185 answerable contact attempts with 25,524 contacts answered
- Kids Helpline received 240,823 answerable contact attempts (call, webchat and email) with 136,424 contacts answered.
- Beyond Blue received 303,138 contacts and responded to 228,415 contacts (AIHW, unpublished).
National Disability Insurance Scheme
The NDIS provides support to people with a significant and enduring primary psychosocial disability. As at 30 June 2025, there were 65,272 active NDIS participants with a psychosocial disability (9.0% of all participants), a 2% increase from 30 June 2024 (NDIA 2025), receiving approximately $5.7 billion in payments (table 13A.14).
A PDF of Part E Health can be downloaded from the Part E sector overview page.