Report on Government Services 2026
PART E, SECTION 10: RELEASED ON 5 FEBRUARY 2026
10 Primary and community health
This section reports on the performance of primary and community health services which include general practice, pharmaceutical services, dentistry, allied health services, community health services, maternal and child health and alcohol and other drug treatment. This section does not include:
- public hospital emergency departments and outpatient services (reported in section 12, ‘Public hospitals’)
- community mental health services (reported in section 13, ‘Services for mental health’)
- home and community care services (reported in section 14, ‘Aged care’ and section 15, ‘Services for people with disability’).
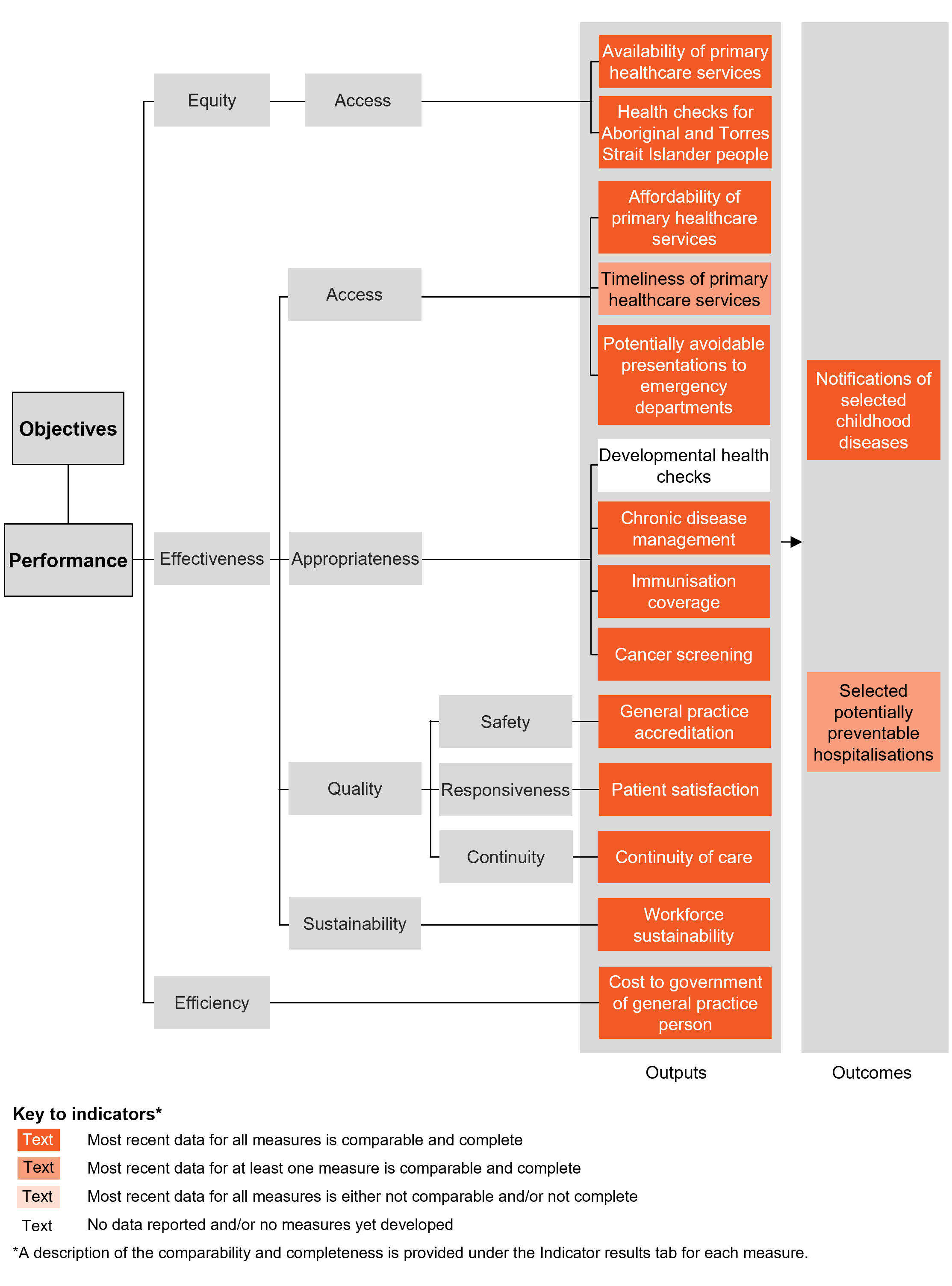
The Indicator results tab uses data from the data tables to provide information on the performance for each indicator in the Indicator framework. The same data is also available in CSV format.
Data downloads
- 10 Primary and community health data tables (Excel - 1000.2 KB)
- 10 Primary and community health dataset (CSV - 3.3 MB)
Refer to the corresponding table number in the data tables for detailed definitions, caveats, footnotes and data source(s).
Context
Objectives for primary and community health
Primary and community health services aim to promote health, prevent illness and support people to manage their health issues in the community, by providing services that are:
- timely, affordable and accessible to all
- appropriate and responsive to meet the needs of individuals throughout their lifespan and communities
- well coordinated to ensure continuity of care where more than one service type, and/or ongoing service provision is required
- sustainable.
Governments aim for primary and community health services to meet these objectives in an equitable and efficient manner.
Primary and community health services are delivered by a range of health and allied health professionals across private, not‑for‑profit and government service settings. Definitions for common health terms are provided in the 'Explanatory material' tab.
General practice
General practice is a major provider of primary healthcare in Australia. Services include preventative care, the diagnosis and treatment of illness and injury, delivered directly and/or through referral to acute (hospital) or other healthcare services.
The Australian Government provides the majority of general practice income, through Services Australia – mainly as fee-for-service payments via the Medicare Benefits Schedule (Medicare) – and the Department of Veterans’ Affairs (DVA). Additional funding is provided to influence the supply, regional distribution and quality of general practice services, and support engagement of the health workforce in primary health care settings including residential aged care. This includes initiatives such as the Practice Incentives Program, the Workforce Incentive Program, the General Practice in Aged Care Incentive and Primary Health Networks (Services Australia 2025). State and territory governments also provide some funding for such programs, mainly to influence the availability of General Practitioners (GPs) in rural and remote areas. Other funding sources include insurance schemes (for example, workers compensation and traffic accident schemes) and patient contributions.
Pharmaceutical services
The Australian Government funds the Pharmaceutical Benefits Scheme (PBS), which subsidises the cost of many medicines in Australia. The PBS schedule sets a price for listed medicines and a maximum co-payment amount that people contribute towards the cost of these medicines. The Australian Government incurs the expense of any difference where the listed price exceeds the patient co-payment (whether for general or concessional patients).
In 2022-23, around 69% of PBS prescriptions dispensed were above the co-payment threshold. Patients paid the co-payment and Australian Government subsidised the remainder. Around 31% were below the threshold, meaning the patient paid the full cost with no government subsidy (AIHW 2024a). Co-payments contribute to a patient’s safety net threshold that, once reached, provides eligibility to receive PBS medicines at a lower cost or free of charge (DHDA 2025a).
The Repatriation Pharmaceutical Benefits Scheme (RPBS) provides subsidised pharmaceutical medicines, dressings and other items to war veterans and war widows. The RPBS is administered by the DVA.
Dental services
Australia has a mixed system of public and private dental services. State and territory governments deliver public dental services, which are primarily available to children and disadvantaged adults. The Australian Government works with state and territory governments to fund dental services. Since 2013, the Australian Government has increased funding for public dental services via National Partnership Agreements and Federal Funding Agreements with states and territories and the Child Dental Benefits Schedule. The private sector receives funding to provide some public dental services from the Australian Government through the DVA and the Child Dental Benefits Schedule, and from state and territory governments through dental voucher systems. The Australian Government is working with states and territories to develop the next ten-year National Oral Health Plan which will set out priorities to improve dental health across Australia (DHDA 2025b). Data on dental service expenditure for the years 2014-15 to 2023-24 is presented in table 10A.6.
Allied health services
Allied health services include, but are not limited to, physiotherapy, psychology, occupational therapy, podiatry and osteopathy. They are delivered mainly in the private sector. Some government funding of private allied health services is provided through insurance schemes and the private health insurance rebate. The Australian Government makes some allied health services available under Medicare to patients with particular needs – for example, people with chronic conditions and complex care needs. The Australian Government also funds the Workforce Incentive Program – Practice Steam, which supports general practices, Aboriginal Medical Services and Aboriginal Community Controlled Health Services with the cost of engaging eligible allied health professionals. Data on the number of Medicare rebated allied health services used per person and the availability of public allied health professionals by region is presented in tables 10A.10 and 10A.22, respectively.
Community health services
Community health services generally comprise multidisciplinary teams of health and allied health professionals who provide targeted health promotion, prevention and management services. Their aim is to protect the health and wellbeing of local populations, particularly people who have or are at risk of the poorest health and/or have the greatest economic and social needs, while taking pressure off the acute care health system. Governments (including local governments) provide community health services directly or indirectly by funding local health services and community organisations. There is no national strategy for community health services and service provision varies across jurisdictions.
State and territory governments are responsible for most community health services. The Australian Government is primarily responsible for serving Aboriginal and Torres Strait Islander communities, with state and territory governments also providing some funding.
Maternal and child health services
Maternal and child health services are funded by state and territory governments. They provide services including: parenting support (including antenatal and postnatal programs); early childhood nursing programs; disease prevention programs (including childhood immunisations); and early intervention and treatment programs related to child health and development. Some jurisdictions also provide specialist programs through child health services, including hearing screening programs, and mothers and babies residential programs.
Alcohol and other drug treatment
Alcohol and other drug treatment activities range from a brief intervention to long-term residential treatment. Types of treatment include withdrawal management, pharmacological treatment, counselling and rehabilitation. Selected data on these services is available in table 10A.13.
In 2023-24, of the $51.5 billion government recurrent expenditure on primary and community health services, almost three-quarters was funded by the Australian Government and one-quarter by state, territory and local governments (table 10A.1). This included:
- $12.8 billion for community health services (16.5% by the Australian Government and 83.5% by state, territory and local governments)
- $2.5 billion for dental services (57.9% by the Australian Government and 42.1% by state, territory and local governments) (table 10A.6).
Where more recent data is available, for 2024-25, Australian Government expenditure was:
- $13.4 billion on general practice (table 10A.2)
- $19.5 billion through the PBS and RPBS on Section 85 prescription medicines filled at pharmacies (table 10A.3). Expenditure by type of service is available in table 10A.4
- $70.5 million on funding of PBS medicines to Aboriginal and Torres Strait Islander primary health services in remote and very remote areas (table 10A.5)
- $981.0 million on Aboriginal and Torres Strait Islander primary health services (table 10A.7).
Nationally in 2024, there were 40,375 GPs – 29,976 on a full-time equivalent (FTE) basis, equating to 110.2 GPs per 100,000 people (table 10A.8), similar to 109.7 in 2023. This remains lower than the peak in 2021 (120.9) (table 10A.8).
Nationally in 2024-25, rates of GP-type services used per person was 6.4 services per person, similar to 2023-24 (6.3 services per person) (figure 10.1). GP-type services disaggregated by in-person attendances and telehealth appointments are reported in table 10A.9. Nationally in 2024-25, 1.0 telehealth GP-type service was used per person (table 10A.9).
In 2024-25, around 226 million services (8.2 per person) were subsidised under Section 85 of the PBS with 87.0% provided to concessional patients. A further 6.9 million services were subsidised under the RPBS (tables 10A.11–12).
Nationally in 2023-24 there were:
- 1,304 alcohol and other drug treatment agencies (31.2% identified as government providers) with a reported 240,958 closed treatment episodes (26.8% identified as government provided) (table 10A.13).
- 213 Aboriginal and Torres Strait Islander primary health services which provided 3.8 million episodes of healthcare (table 10A.14). Data by remoteness is presented in table 10A.15 and health service staffing numbers are provided in table 10A.16.
The most recent available data on public dental service usage (2021) showed that nationally, 11% of adults aged 18 years or over visited a public dental practice for their last dental visit (AIHW 2024b).
A PDF of Part E Health can be downloaded from the Part E sector overview page.


Measure 2: Nationally in 2024-25, for people who saw a GP for urgent care:
Overall, nationally in 2024-25, 26.0% of people who saw a GP for their own health waited longer than they felt was acceptable to get an appointment, a decrease on 2023-24 (28.0%), although a 9.1 percentage point increase across the time series (18.9% in 2015-16) (table 10A.44).